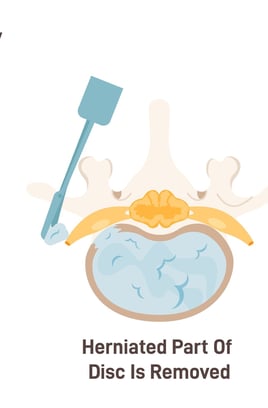
Approximately 500,000 discectomies are performed annually in the US to address IVD herniation.
Discectomy mechanically removes herniated NP and AF fragments; however the defect pathway in the IVD remains unrepaired.
The defect pathway fills with unorganized, mechanically weak scar tissue.3
The multilaminate, angle-ply microarchitecture and strength of the AF is not re-established.
Reherniation rates of up to 25% have been reported in patients with large (≥6mm) defects.4


IVD Herniation:
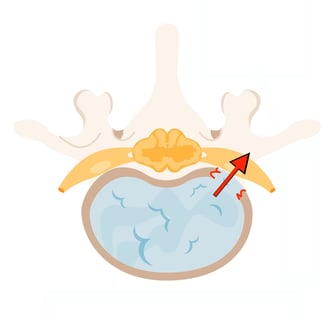
Occurs when the NP protrudes or extrudes from the restraint of the AF.
Results in significant pain, disability, altered spine biomechanics and reduced quality of life.
Affects over 3-million new patients each year in the US.1
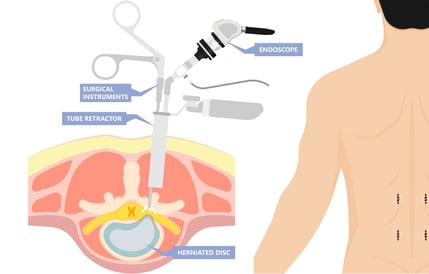
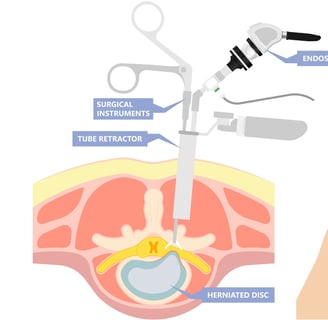
A CRITICAL NEED EXISTS for a device that mimics the structure and function of the native AF that can quickly and immediately restore AF integrity, while allowing for tissue integration and remodeling to reduce the incidence of reherniation following discectomy.
Repair of Annular Defects Improve Patient Outcomes
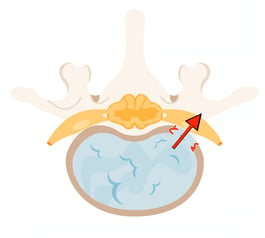
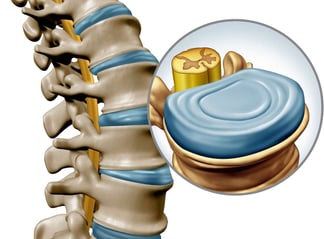
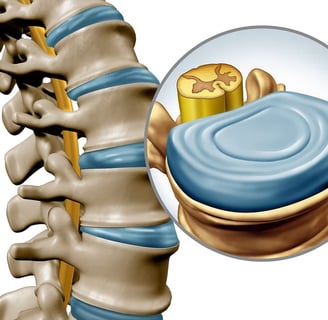
The Intervertebral Disc
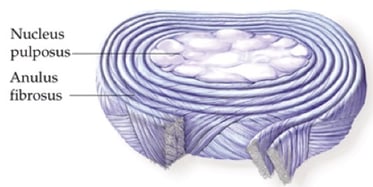
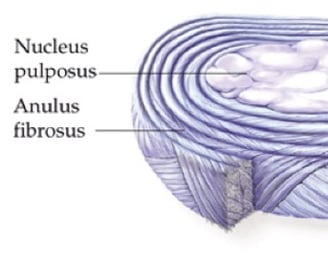
Herniation Impacts Millions of Patients Globally and Results in a Mechanically Compromised Disc
Discectomy Surgery Relieves Pain but Leaves Patients at Risk for Reherniation
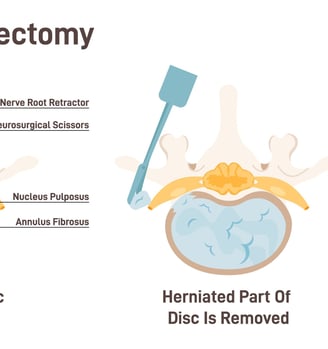
The intervertebral disc (IVD) is composed of a centrally-located gelatinous core known as the nucleus pulposus (NP).
The NP is circumferentially restrained by 15-20 concentric layers of type 1 collagen known as the annulus fibrosus (AF).
Collagen fibers in the AF alternate at ±30 degrees to the horizontal axis of the spine in consecutive layers forming a multilaminate angle-ply microarchitecture.
Repair of Annular Defects Results In:
52% reduction in reherniation rates,
62% reduction in reoperation rates, and
Reduced pain compared to discectomy alone.5
Current Repair Devices DO NOT Restore AF Structure, Function, or Integrate with Native IVD Tissue!


REFERENCES
1 McCulloch JA. Focus issue on lumbar disc herniation: macro- and microdiscectomy. Spine (Phila Pa 1976). 1996; 21(24 (Suppl.):45S-56S.
2 Gray DT, Deyo RA, Kreuter W, et al. Population-based trends in volumes and rates of ambulatory lumbar spine surgery. Spine (Phila Pa 1976). 2006;31(17):1957-1963.
3 Li X, Dou Q, Kong Q. Repair and regenerative therapies of the annulus fibrosus of the intervertebral disc. Journal of the College of Physicians and Surgeons Pakistan. 2016;26(2):138-144.
4 Choy WJ, Phan K, Diwan AD, Ong CS, Mobbs RJ. Annular closure device for disc herniation: Meta-analysis of clinical outcome and complications. BMC Musculoskelet Disord. 2018;19(1):1-9.
5 Thomé C, Klassen PD, Bouma GJ, et al. Annular closure in lumbar microdiscectomy for prevention of reherniation: a randomized clinical trial. Spine Journal. 2018;18(12):2278-2287.